New Cholesterol Drug Cuts Heart Attack Risk by 31%: A Game-Changer for Heart Health?
Heart disease is still the leading cause of death in the United States; about one in every three deaths in the U.S. comes from cardiovascular causes. What makes this even more concerning is that many of these deaths could be prevented with the right care and treatment. Now, there’s some encouraging news. A new clinical study released just a few days ago is getting a lot of attention from heart experts. It focuses on a cholesterol-lowering drug called “Evolocumab” (brand name Repatha). The study found something remarkable: this medication can reduce the risk of a first heart attack or stroke by 31%. This is especially important for people with diabetes who are at high risk but haven’t yet shown clear signs of blocked arteries.
In simple terms, this means doctors may have a powerful new way to stop serious heart problems before they even start. For millions of people living with diabetes, this could be a game-changer in protecting long-term heart health.
Table of Contents
What Is the New Heart Drug?
The medication currently making headlines is “Evolocumab”, a PCSK9 inhibitor available on the market under the brand name “Repatha”. Unlike traditional medicine, which inhibits cholesterol production in the liver, “Evolocumab” is a biologic therapy administered via subcutaneous injection, typically once every two weeks or once a month, depending on the dosage. It works by targeting a protein called PCSK9, which normally prevents the liver from clearing “bad” LDL cholesterol from the bloodstream. By blocking PCSK9, the liver is able to remove significantly more LDL, thereby dramatically lowering its levels.
This new heart drug 2026 spotlight comes not because of brand new, but because clinical trial results prove its power in an entirely new group, people who haven’t yet had a heart attack or stroke. This shift from secondary prevention to primary prevention represents a major breakthrough. Traditional treatments such as “statins” remain the primary line of therapy; however, many patients are either unable to tolerate the muscle pain and other side effects associated with them, or they fail to achieve sufficiently aggressive LDL targets. In such cases, “Evolocumab” emerges as a potent alternative to “statins”, often utilized in conjunction with “statins” or other therapies such as “Ezetimibe”. While it is not a daily oral pill, for many individuals, the convenience of its injectable format combined with its exceptional clinical outcomes makes it a highly compelling treatment option.
Key Study Findings (The 31% Breakthrough)
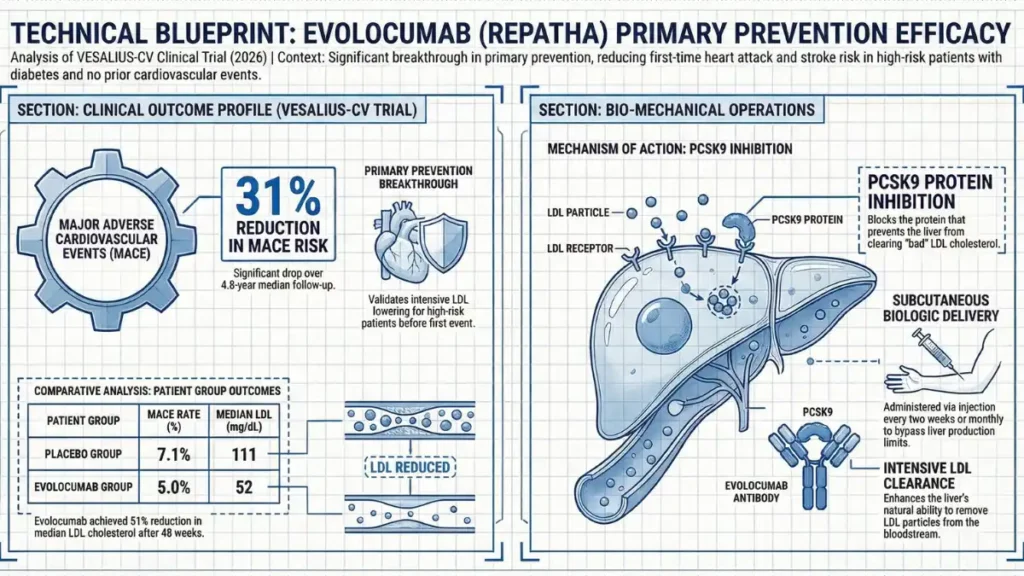
The numbers come from a prespecified subgroup analysis of the VESALIUS-CV trial, led by researchers at Mass General Brigham and presented at the American College of Cardiology’s 2026 Scientific Session. The full trial enrolled over 12,000 high-risk patients without prior heart attacks or strokes. This analysis zeroed in on 3,655 participants with diabetes who were considered high-risk but showed no significant atherosclerosis on imaging or history.
medicines plus Over a median follow-up of nearly five years (about 4.8 years), patients who added “Evolocumab” to their standard therapy (usually statins plus ezetimibe) saw their risk of a first major cardiovascular event drop by 31%. Specifically, the three-point major adverse cardiovascular event (MACE) rate, which includes coronary heart disease death, heart attack, or ischemic stroke, fell from 7.1% in the placebo group to 5.0% in the “Evolocumab” group. The broader four-point MACE (adding ischemia-driven revascularization) showed the same 31% relative risk reduction.
LDL cholesterol plunged too: after 48 weeks, median levels hit 52 mg/dL in the treatment arm versus 111 mg/dL on placebo—a roughly 51% drop. Some later measurements showed even deeper reductions, with median LDL around 44 mg/dL at 96 weeks. Additional benefits included trends toward lower overall mortality. These aren’t small tweaks; they represent a clear cholesterol lowering breakthrough that could prevent thousands of first-time events across the country.
How the Drug Works in the Body
Imagine your liver acting like a powerful vacuum cleaner for cholesterol. PCSK9 is like a faulty switch that keeps telling the vacuum to stop working too soon. “Evolocumab” flips that switch off, letting the liver keep sucking up LDL particles from the blood. he result is cleaner arteries, less sticky plaque buildup, and a big drop in the dangerous inflammation that can suddenly trigger a heart attack or stroke.
Compare that to statins, which mainly slow down cholesterol production in the liver but don’t always clear existing LDL efficiently, especially in people with genetic factors or stubborn high cholesterol. Then, this mechanism works “Evolocumab” a true LDL cholesterol treatment game-changer, achieving levels that were previously difficult or impossible with pills alone. Cardiologists call it “intensive lowering” because it pushes LDL into ranges once thought unnecessary for primary prevention. The breakthrough here is proving that getting LDL that low early, before plaque is even visible, actually reduces heart attack risk in real-world high-risk groups.
Who Could Benefit the Most?
Not everyone needs this level of drug, but certain groups of high-risk people with diabetes, especially those who’ve had the condition for 10 years or more, require daily insulin, or already show microvascular complications like kidney or eye damage. The study focused on folks without known artery disease, so it helps for earlier intervention in the body.
Other group of people includes adults over 40 with persistently high LDL despite maximum statins, those with a family history of early heart disease, or anyone who simply can’t tolerate statins, well. In the U.S., where roughly 100 million adults have high cholesterol and diabetes rates continue climbing, this could touch millions. Think busy professionals in their 50s juggling stress and poor diet, or older adults with multiple risk factors. The data suggest the biggest payoff comes when you start before the first crisis hits.
Is It Safe? Side Effects & Concerns
Serious adverse events occurred at similar rates in both the “Evolocumab” and placebo groups in the trial. Common side effects such as: mild injection-site reactions, occasional cold-like symptoms, or back pain. No major new red flags emerged even after years of use.
Experts emphasize it’s generally well tolerated, though long-term data continues to be monitored. FDA approval for broader primary prevention use is already expanding based on earlier results, and this latest evidence strengthens the case. Cost remains the biggest practical hurdle, PCSK9 inhibitors can run $5,000 or more per year without good insurance coverage, though manufacturer assistance programs and potential biosimilars are helping. Accessibility in the U.S. depends heavily on insurance plans and prior authorization requirements, which can be frustrating. Still, as cardiovascular health news evolves, more payers are recognizing the long-term savings from prevented hospitalizations.
Expert Opinions & Reactions
Cardiologist Nicholas A. Marston, MD, MPH, the study’s corresponding author from Mass General Brigham, put it bluntly: “For over a decade, intensive cholesterol-lowering has been reserved for patients who already have cardiovascular disease. These results demonstrate the benefit of intensive lowering cholesterol earlier and should change how we think about the prevention of heart attacks, strokes, and heart disease in patients without known significant atherosclerosis.”
Other cardiologists echo the excitement. Many see this as validation that “lower is better” when it comes to LDL, especially in diabetes. Public health leaders note the potential to narrow disparities, diabetes hits certain communities harder, so earlier access could save lives equitably. The American College of Cardiology and American Heart Association are already incorporating similar aggressive targets into updated guidelines.

Should You Ask Your Doctor About It?
If you’re over 40 and dealing with high cholesterol, diabetes, or other heart attack-related risk factors, it’s worth having an honest conversation with your doctor about evolocumab (Repatha). This statin alternative drug may offer extra protection, especially if your current treatment isn’t bringing your cholesterol down enough or if you’ve had trouble with statin side effects.
Lifestyle Still Matters
No drug replaces healthy habits. A heart-healthy Mediterranean-style diet rich in vegetables, nuts, and fatty fish can lower LDL naturally. Regular exercise, aiming for 150 minutes of moderate activity weekly, strengthens your heart and improves cholesterol profiles. Quitting smoking is non-negotiable; it damages arteries faster than almost anything else. Weight management, stress reduction, and good sleep round out the picture.
When Will This Drug Be Available?
The good news is that it is already available in the U.S. market. Repatha has been on the market for years, and prescribers can use this new data to justify broader prescribing for high-risk diabetes patients without known atherosclerosis. Insurance coverage is expanding as evidence grows, though patients should check their plan for copays and requirements. Talk to your doctor soon if you fit the profile; no need to wait for a formal “new approval” in many cases.
FAQ
Is this “Evolocumab” drug better than statins?
It’s not “better” for everyone; medicines remain first-line and far cheaper. But for people who need extra LDL reduction or can’t tolerate statins, “Evolocumab” delivers deeper drops and proven event reduction.
How fast does it (“Evolocumab” drug) work?
LDL levels drop noticeably within weeks, but the full protective effect on heart events builds over months to years, as seen in the five-year data.
Conclusion
This 31% risk reduction in first-time heart attacks and strokes isn’t hype; it’s hard data from a rigorous trial that could prevent countless tragedies. The new heart drug 2026 isn’t promising miracles, but it offers a genuine cholesterol-lowering breakthrough for millions at risk. It’s not a free pass to ignore diet or exercise; instead, it’s a powerful partner in heart disease prevention in the USA.
